What is it?
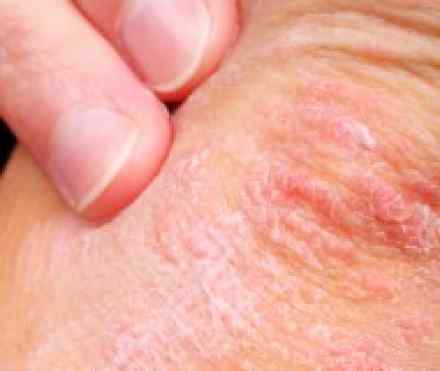
- Dermatitis is a general term that describes an inflammation of the skin. There are different types of dermatitis, including seborrheic dermatitis and atopic dermatitis (eczema). Although the disorder can have many causes and occur in many forms, it usually involves swollen, reddened and itchy skin.
- Dermatitis is a common condition that usually isn't life-threatening or contagious. But, it can make you feel uncomfortable and self-conscious. A combination of self-care steps and medications can help you treat dermatitis.
Symptoms
There are several types of dermatitis, including:
- Contact dermatitis, a rash that results from either repeated contact with irritants or contact with allergy-producing substances, such as poison ivy
- Neurodermatitis, a chronic itchy skin condition localized to certain areas of the skin
- Seborrheic dermatitis, a common scalp and facial condition that often causes dandruff
- Stasis dermatitis, a skin condition that's caused by a buildup of fluid under the skin of the legs
- Atopic dermatitis, more commonly known as just eczema or atopic eczema, a chronic itchy rash that tends to come and go
- Perioral dermatitis, a bumpy rash around the mouth
Each has distinct signs and symptoms. Common signs and symptoms include:
- Redness
- Swelling
- Itching
- Skin lesions
Causes
A number of health conditions, allergies, genetic factors, physical and mental stressors, and irritants can cause dermatitis.
Contact dermatitis
This condition results from direct contact with one of many irritants or allergens.
Common irritants include:
- Laundry soap
- Skin soaps or detergents
- Cleaning products
Possible allergens include:
- Rubber
- Metals, such as nickel; jewelry
- Perfume and fragrances
- Cosmetics
- Weeds, such as poison ivy
- Neomycin, a common ingredient in topical antibiotic creams
It takes a greater amount of contact with an irritant over a longer time to cause dermatitis than it takes for an allergen. Once you're sensitized to an allergen, just brief exposure to a small amount of it can cause dermatitis. Once you develop sensitivity to an allergen, you typically have it for life.
Neurodermatitis
This type of dermatitis typically develops when something has created an itchy sensation in a specific area of your skin. This irritation may lead you to rub or scratch your skin repeatedly in that area. Common locations include ankles, wrist, outer forearm or arm, and the back of your neck.
Possible causes include:
- Dry skin
- Chronic irritation
- Eczema
- Psoriasis
Seborrheic dermatitis
This condition causes a red rash with yellowish and somewhat "oily" scales, usually on the scalp. It's common in people with oily skin or hair, and it may come and go depending on the season of the year. It's likely that hereditary factors play a role in this condition.
Possible causes include:
- Physical stress
- Travel
- Neurological conditions, such as Parkinson's disease
- In infants, this disorder is known as cradle cap.
Stasis dermatitis
Stasis dermatitis can occur when fluid accumulates in the tissues just beneath the skin — typically on your lower legs — due to a sluggish return of blood from the leg veins back to the heart. The extra fluid interferes with your blood's ability to nourish your skin and places extra pressure against your skin from underneath.
Possible causes include:
- Varicose veins
- Other chronic conditions or recurrent infections that affect circulation in your legs
Atopic dermatitis
This condition often occurs with allergies and frequently runs in families in which members have asthma or hay fever. It usually begins in infancy and may vary in severity during childhood and adolescence. It tends to become less of a problem in adulthood, unless you're exposed to allergens or irritants in the workplace.
Possible causes include a combination of:
- Dry, irritable skin
- A malfunction in the body's immune system
- A genetic tendency for allergic conditions such as asthma or hay fever
Stress can exacerbate atopic dermatitis, but it doesn't cause it.
Perioral dermatitis
This type of dermatitis may be a form of the skin disorder rosacea, adult acne or seborrheic dermatitis, involving the skin around the mouth or nose.
Possible causes include:
- Makeup
- Moisturizers
- Topical corticosteroids
- Dental products containing fluoride
Complications
- Impetigo. The open sores and fissures that can occur with dermatitis may become infected. A mild form of infection is impetigo, usually due to staphylococci bacteria. Having atopic dermatitis predisposes you to this infection.
- Cellulitis. If you notice red streaks on your skin, you may have cellulitis, a bacterial infection of tissues under the skin. Cellulitis appears as intensely inflamed skin that's swollen, red, tender and warm to the touch, with spreading, indistinct margins. Cellulitis that occurs in someone whose immune system is compromised is potentially life-threatening. See your doctor as soon as possible if you think you have cellulitis.
Scarring and changes in skin color are other potential complications from dermatitis.
Diagnosis
Your doctor may diagnose dermatitis after talking to you about your signs and symptoms and examining your skin.
Patch testing
In the case of contact dermatitis, your doctor may conduct patch testing on your skin to see which substances inflame your skin. In this test, your doctor applies small amounts of various substances to your skin under an adhesive covering. During return visits over the next several days, your doctor examines your skin to see if you've had a reaction to any of the substances. This type of testing is most useful for determining if you have specific contact allergies.
Treatments and drugs
Dermatitis treatment varies, depending on the cause. Corticosteroid creams, wet compresses and avoiding irritants are the cornerstones of most dermatitis treatment plans. To minimize side effects, such as thin skin, and to increase effectiveness, topical corticosteroids are generally used only short-term until rashes are under control.
For some types of dermatitis, nonsteroidal medications may help relieve signs and symptoms. And for all types of dermatitis, occasional use of over-the-counter antihistamines can reduce itching.
Contact dermatitis
Treatment consists primarily of identifying the cause of the rash and then avoiding it.
Treatment options include:
- Creams containing hydrocortisone
- Other, stronger steroidal creams
- Wet dressings applied over steroid creams
Neurodermatitis
Getting you to stop scratching and to avoid further aggravating your skin are the treatment objectives.
Treatment options include:
- Covering the affected area to prevent you from scratching it
- Hydrocortisone and similar lotions and creams
- Wet compresses
- In some cases, antidepressants or anti-anxiety medications
In addition, counseling can help you learn how your emotions and behaviors can fuel — or prevent — itching and scratching.
Seborrheic dermatitis
Medicated shampoos are usually the first treatment choice.
Treatment options include:
- Shampoos that contain tar, pyrithione zinc, salicylic acid or ketoconazole as the active ingredient
- Hydrocortisone creams and lotions for nonscalp seborrheic dermatitis
- Nonsteroidal medications called immunomodulators
Immunomodulators, such as tacrolimus (Protopic) and pimecrolimus (Elidel), affect the immune system and have anti-inflammatory and mild antifungal properties.
Due to possible concerns about the effect of prolonged use of these medications on the immune system, the Food and Drug Administration recommends that Elidel and Protopic be used only when other treatments have failed, or if someone can't tolerate other treatments.
Stasis dermatitis
Treatment consists of correcting the condition that causes fluid to accumulate in your legs or ankles for extended periods.
Treatment options include:
- Wearing elastic support hose
- Having varicose vein surgery
- Using wet dressings to soften the thickened yet fragile skin and to control infection
Atopic dermatitis
In addition to relieving redness and itching, treatments for this condition are aimed at healing infection-prone cracks in your skin.
Treatment options include:
- Hydrocortisone-containing lotions
- Wet dressings with mildly astringent properties
- Immunomodulator drugs, such as tacrolimus (Protopic) and pimecrolimus (Elidel)
In addition, light therapy, which involves exposing your skin to controlled amounts of natural or artificial light, may be used to help prevent recurrences of atopic dermatitis.
Perioral dermatitis
In general, doctors try to avoid treating this condition with strong corticosteroids. When these potent medications are stopped, perioral dermatitis may return and even worsen.
Treatment options include:
- The oral antibiotic tetracycline, often taken for several months
- A mild corticosteroid cream
Lifestyle remedies
These steps can help you manage dermatitis:
- Apply an anti-itch cream or calamine lotion to the affected area. A nonprescription hydrocortisone cream, containing at least 1 percent hydrocortisone, can temporarily relieve your itch. A nonprescription oral antihistamine, such as diphenhydramine (Benadryl, others), may be helpful if your itching is severe.
- Apply cool, wet compresses. Covering the affected area with bandages and dressings can help protect your skin and prevent scratching.
- Take a comfortably cool bath. Sprinkle your bath water with baking soda, uncooked oatmeal or colloidal oatmeal — a finely ground oatmeal that's made for the bathtub (Aveeno, others).
- Avoid scratching whenever possible. Cover the itchy area with a dressing, if you can't keep from scratching it. Trim nails and wear gloves at night.
- Wear smooth-textured cotton clothing. This will help you avoid irritating the affected area.
- Use a mild, unscented laundry detergent when washing clothes, towels and bedding. Try using the extra-rinse cycle on your wash machine.
Alternative medicine
A number of natural options have been studied as possible treatments for dermatitis. Although none are as potent as steroid medications, natural approaches generally aren’t associated with the same risk of side effects. These therapies also don’t carry the risk that symptoms may return and even worsen once you stop using them.
You may wish to talk with your doctor about natural therapies for dermatitis, including:
- Evening primrose oil. This oil is a form of linoleic acid that's available as an over-the-counter supplement. Evening primrose oil may benefit atopic dermatitis by improving deficient levels of essential fatty acids. Results from studies of this supplement in the treatment of atopic dermatitis have been conflicting.
- Omega-3 fatty acids. These nutrients, found in fish oil and flaxseed, have anti-inflammatory properties and may help improve skin rashes.
- Chamomile creams. Studies have found that topical chamomile is about as potent as a product containing 0.25 percent hydrocortisone. Chamomile-based creams may help relieve dermatitis.
- Calendula creams. Calendula has skin-soothing properties and may protect against contact dermatitis. However, it may trigger an allergic reaction on broken skin, so is not safe to use when your skin is cracked.
Prevention
Preventing contact dermatitis means avoiding coming into contact with those substances, such as poison ivy or harsh soaps, that may cause it.
Try to identify and avoid triggers that worsen the inflammation. Rapid changes of temperature, sweating and stress can worsen some forms of dermatitis. Avoid direct contact with wool products, such as rugs, bedding and clothes, as well as harsh soaps and detergents. If you must handle products that irritate your skin, wear nonlatex gloves.
Avoiding dry skin may be one factor in helping you prevent future bouts of dermatitis. These tips can help you minimize the drying effects of bathing on your skin:
- Bathe less frequently. Most people who are prone to dermatitis don't need to bathe daily. Try going a day or two without a shower or bath. When you do bathe, limit yourself to 15 to 20 minutes, and use warm, rather than hot, water.
- Use only mild soaps. Choose soaps, such as Basis, Dove or Olay, that clean without excessively removing natural oils. Deodorant and antibacterial soaps may be more drying to your skin. Use soap only on your face, underarms, genital areas, hands and feet. Use clear water elsewhere.
- Dry yourself carefully. Brush your skin rapidly with the palms of your hands, or gently pat your skin dry with a towel after bathing.
- Moisturize your skin. Seal in moisture, while your skin is still damp, with an oil or cream. Pay special attention to your legs, arms, back and the sides of your body. If your skin is already dry, consider using a lubricating cream made for dry skin, such as Eucerin.
References:
http://www.dermnetnz.org/dermatitis/dermatitis.html
http://www.healthline.com/health/contact-dermatitis
https://en.wikipedia.org/wiki/Dermatitis
https://nationaleczema.org/eczema/types-of-eczema/seborrheic-dermatitis/